Search VernonNow
How many people are overdosing while they are patients at British Columbia’s hospitals?
This data is essential to understanding the importance of opening hospital-based overdose prevention sites, addiction medicine doctors told The Tyee.
In an atmosphere where the province’s drug policy is a hot-button topic, it’s also key to developing public understanding about why the sites are necessary, doctors added. This is because it is safer for both patients and staff when patients who use substances are able to use them at adjacent overdose prevention sites, rather than feeling pressure to either be discharged early or use substances illicitly in places where they can find privacy, such as hospital bathrooms.
But after seven months, seven freedom of information requests and two Office of the Information and Privacy Commissioner complaints, The Tyee is no closer to a strong understanding of how many people are currently surviving overdoses as patients in hospitals across B.C.

In late 2024, addiction medicine doctors started opening unsanctioned overdose prevention sites outside of hospitals in Nanaimo and Victoria where they worked.
These sites were necessary because between 25 and 50 patients at every major B.C. hospital used unregulated drugs and benefited from being able to access an overdose prevention site, Dr. Jess Wilder told The Tyee at the time.
The toxic drug crisis has been considered a public health emergency in B.C. since April 2016. From January 2014 to October 2025, the most recent date for which data is available, more than 18,752 British Columbians died due to unregulated drugs.
Wilder, who was a family and addiction medicine doctor in Nanaimo, resigned after alleged backlash from her employer over her advocacy work.
In late 2024, Island Health said it did not need overdose prevention sites at its hospitals. Island Health did not allow the doctors to set up unsanctioned sites on hospital grounds.
By June 2025, however, B.C.’s Health Ministry said it was directing health authorities to open more overdose prevention sites at hospitals.
In a press release, it quoted doctors saying overdose prevention sites “significantly reduced harms from overdoses for patients and visitors” and were a “great addition” to the emergency department.
Nine B.C. hospitals were already running overdose prevention sites, the press release said.
B.C. is home to 113 hospitals. So what did the data say about patient overdoses at the remaining 104 hospitals? Would they benefit from adjacent overdose prevention sites, too?
Here at The Tyee, we wanted to know more.
The data we were able to access
On June 30, 2025, The Tyee filed freedom of information or FOI requests with Vancouver Coastal Health, Fraser Health, Interior Health, Northern Health, Island Health, Providence Health Care and the Provincial Health Services Authority, asking for a breakdown of the number of fatal and non-fatal overdoses, per hospital, over the last five years.
We also asked the health authority to note when and where overdose prevention sites had opened so we could compare fatalities before and after the sites had opened.
We did not file an FOI request with the First Nations Health Authority because it does not directly oversee any hospitals in B.C.
Within about a week, the health authorities had all gotten back to us, assigning each request a case number and noting how the Freedom of Information and Protection of Privacy Act required them to respond to the request within 30 business days.
Three health authorities asked The Tyee to pay a $10 fee for the FOI, which we paid. Four did not ask for money.
The Provincial Health Services Authority, or PHSA, and Providence Health Care released the requested data.
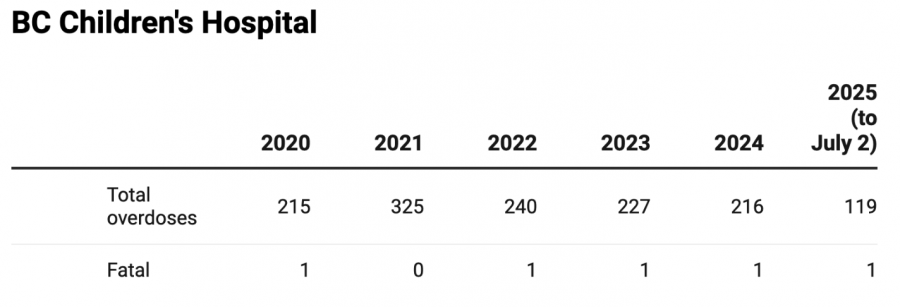
The PHSA reported all overdose calls for drugs or alcohol at BC Children’s Hospital, grouping together inpatient data with data for patients who were brought to the emergency department for an overdose.
PHS Community Services Society ran a mobile overdose prevention site at BC Women’s Hospital from March 16 to Sept. 15, 2023, which is on the same campus as BC Children’s Hospital.
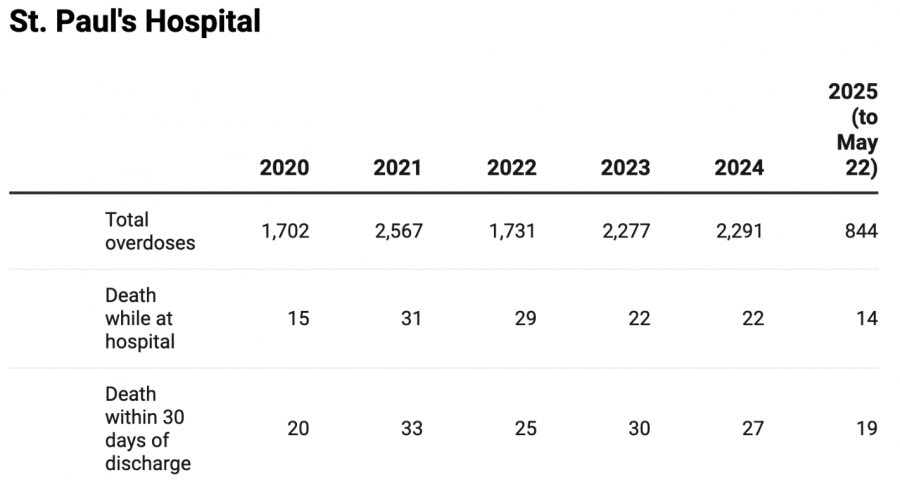
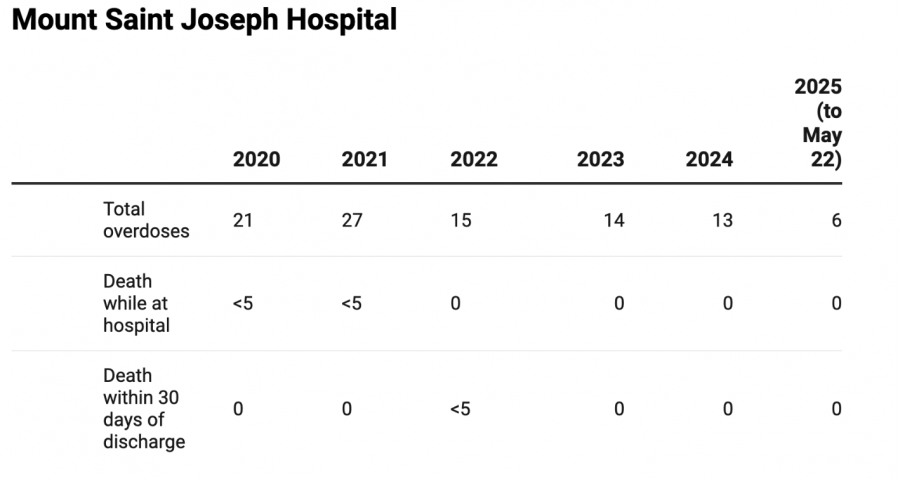
Providence Health’s numbers included only opioid-related overdoses from Jan. 1, 2020, to July 31, 2025, which means overdoses from other drugs such as stimulants and benzodiazepines, alcohol or other non-opioid drugs were excluded. However, toxicology reporting from the BC Coroners Service highlights how the overdose crisis is being driven by fentanyl, with more than 84 per cent of deaths involving fentanyl in 2024.
Providence Health’s data also grouped together inpatient data with data for patients who were brought to the emergency department for an overdose.
An overdose prevention site opened at St. Paul’s Hospital in 2021.
The deaths listed in this data may be related to but are not necessarily caused by an overdose, as the BC Coroners Service has the sole authority to determine whether a death was caused by an overdose after an investigation.
The Tyee asked the coroners service for a list of overdose fatalities in B.C. hospitals since January 2020.
According to the BC Coroners Service, since January 2020, there have been 18 overdose deaths at St. Paul’s, one at Mount Saint Joseph Hospital and one at BC Children’s and Women’s Hospital.
.png)
Vancouver Coastal Health and Interior Health refused to release any data.
Both health authorities said the amalgamated data would amount to an “unreasonable invasion” of a patient’s personal privacy, especially in cases where there were fewer than five non-fatal overdoses at a single hospital in a year.
Vancouver Coastal Health also said non-fatal overdoses are reported in its Patient Safety and Learning System, which is reviewed by a committee and is therefore exempt from being accessed through a freedom of information request.
Interior Health said that reporting non-fatal overdoses is voluntary and the data is therefore exempt from being accessed through a freedom of information request.
Northern Health, Fraser Health and Island Health never officially responded to The Tyee’s freedom of information request beyond assigning the request a case number and noting it had a 30-day legislated response time.
When The Tyee followed up by email in January, Fraser Health said there had been an “internal communication error” that delayed the request. The Tyee has not yet received an updated response.
Northern Health said it forgot to tell The Tyee the request should be forwarded to the BC Coroners Service. When The Tyee responded that only Northern Health could report non-fatal overdose numbers, a spokesperson for the health authority said they would look into it. The Tyee has not yet received an updated response.
Island Health never responded to The Tyee’s followup email.
What the information and privacy commissioner ruled
The Tyee tried to push back against Vancouver Coastal Health and Interior Health’s decisions. We maintained that amalgamated data for an entire year would not be personally identifying and therefore would not violate a patient’s right to privacy.
We filed two complaints to the Office of the Information and Privacy Commissioner, or OIPC, in November 2025, asking them to review the FOI requests and the health authorities’ refusal to release the data.
The Tyee argued again that the amalgamated data didn’t violate patient privacy, making the point that the PHSA and Providence Health had released it, and adding that it was important for the public to know how many people were or were not dying from overdose as hospital patients.
We also argued that if data on fatal overdoses was publicly available, then data on non-fatal overdoses should be too.
The OIPC sided with Interior Health in a December 2025 decision, saying amalgamated data could “reasonably lead to the identification of individuals through the mosaic effect,” where “separate data points, combined with other publicly available or known information, could result in the re‑identification of individuals.”
It added that one health authority releasing amalgamated data does not obligate another to do so.
The Tyee waited two additional months to see if our complaint against Vancouver Coastal Health would have a different outcome.
Finally, we followed up by email. The OIPC responded by saying it had accidentally closed both files after the December decision in favour of Interior Health.
The OIPC said it would look into The Tyee’s complaint against Vancouver Coastal Health and get back to us. The Tyee has not yet received an updated response.
The Tyee then contacted the Health Ministry, laying out why we wanted data on non-fatal overdoses and what work we’d done to try to get it.
We asked the ministry to provide aggregated data on a provincial level — something that surely couldn’t violate patient confidentiality.
In an emailed response, the ministry said: “This request is best answered through the FOI process via the health authorities which it sounds like you’ve already gone through. The ministry has nothing further to add.”
Again, The Tyee pressed, writing that if the ministry wouldn’t release the data, then it should at least offer an explanation as to why it was acceptable to withhold this data during a public health emergency that had killed thousands of British Columbians.
It’s been four weeks and we still haven’t heard back.
Dr. Ryan Herriot, a family doctor and addiction medicine specialist on Vancouver Island, told The Tyee he was surprised and disappointed that the government had not released data on non-fatal overdoses.
“The public has the right to understand these things fulsomely so that we can have informed conversations about policy responses,” he said.
Herriot is the co-founder of Doctors for Safer Drug Policy, the group that opened unsanctioned overdose prevention sites in 2024 and throughout 2025.
“I do not see how this [data on non-fatal overdoses] would violate privacy, especially when talking about aggregate numbers over the course of a year,” he said. “Unless you were providing it week by week, I don’t see how it could possibly be correlated with other pieces of information. I don’t understand that.”
The government’s 2025 press release about opening more overdose prevention sites in hospitals made it “clear” that the province understands these sites are evidence-based, life-saving interventions that improve working conditions for hospital staff and help retain patients in care, Herriot said.
That makes the refusal to release the data on non-fatal overdoses all the stranger, Herriot said.